 |
 |
- Search
| Clin Shoulder Elb > Volume 26(1); 2023 > Article |
|
Abstract
Background
Modifications of the medialized design of Grammont-type reverse shoulder arthroplasty (RSA) using a bony increased offset (BIO-RSA) has shown better clinical results and fewer complications. The aim of this study is to compare the clinical results, complications, and radiological outcomes between patients undergoing standard RSA and BIO-RSA.
Methods
A retrospective review was performed of 42 RSA procedures (22 standard RSA and 20 BIO-RSA). With a minimum of 1 year of follow-up, range of motion (ROM), Constant shoulder score (CSS), visual analog scale (VAS), and subjective shoulder score (SSS) were compared. Radiographs and computed tomography (CT) scan were examined for scapular notching, glenoid and humeral fixation, and graft healing.
Results
At a mean follow-up of 27.6 months (range, 12â48 months), a significant difference was found for active-internal rotation (P=0.038) and for passive-external rotation (P=0.013), with better results in BIO-RSA. No other differences were found in ROM, CSS (P=0.884), VAS score, and SSS. Graft healing and viability were verified in all patients with CT scan (n=34). The notching rate was 28% in the standard RSA group and 33% in the BIO-RSA group, but the standard RSA had more severe notching (grade 2) than BIO-RSA (P=0.039). No other significative differences were found in glenoid and humeral fixation.
Reverse shoulder arthroplasty (RSA) is an effective and safe solution in the treatment of degenerative shoulder disease. Inferior notching of the scapula, prosthetic instability, limitation of shoulder range of motion (ROM), and loss of shoulder contour have been reported and largely attributed to the medialized design of Grammont-type RSA. Modifications to the standard prosthetic design, such as lateralization of the glenosphere, has shown better results in cadaveric studies [1,2], biomechanical works [3,4], and virtual simulation models [5,6].
Technically, lateralization of the rotation center can be performed using metal or bony approaches. However, metallic lateralization results in increased joint loading (compressive and shearing forces) with increased potential for glenoid loosening [7]. The bony increased-offset RSA (BIO-RSA) technique, although still medializing the center of rotation in comparison with the native shoulder, lateralizes the center of rotation in comparison with the standard Grammont technique.
The main advantage of using a bone graft is that the center of rotation remaining at the bone-implant interface reduces the torque forces compared to those with metallic implants, potentially resulting in a more stable construct [8]. In 2011, Boileau et al. [9] published the first study of short-term clinical outcomes of BIO-RSA, and in 2020, the authors published the results of a 5-year follow-up [8]. Other works [10-12] have demonstrated lower rates of scapular notching and instability while allowing greater shoulder mobility in rotation compared with standard RSA.
However, few studies have comparatively evaluated clinical outcomes and rotational function, as well as radiological outcomes by computed tomography (CT) scan, between patients with lateralized BIO-RSA and standard RSA [10-12]. The aim of this study is to compare the clinical results, complications, and radiological outcomes between patients undergoing standard RSA or lateralization with bony increased offset. The authors hypothesize that lateralization results in more effective bone graft integration and better functional results.
The protocol was approved by the Institutional Review Board of the Centro Hospitalar UniversitĂĄrio do Porto and informed consent was obtained.
A retrospective review was performed at a single institution between January 2017 and December 2020 to compare standard RSA with BIO-RSA. Inclusion criteria were primary RSA with preoperative diagnosis of cuff tear arthropathy, massive rotator cuff tear, failed rotator cuff repair, primary osteoarthritis, or rheumatoid arthritis. A minimum of 1 year of follow-up was mandatory. Patients with fracture sequelae, history of infection, shoulder neoplasm, prior open shoulder surgery, or presence of neurologic problems, such as Parkinson disease or axillary nerve lesion, were excluded.
All surgical procedures were performed by two shoulder surgeons (LHB and RC). The Aequalis Ascend Flex Convertible Shoulder System (Wright Medical) was used for both the standard RSA and the BIO-RSA (Fig. 1). All surgical procedures were conducted through a deltopectoral approach in the beach-chair position. The subscapularis or its remnants were detached from the lesser tuberosity with a âpeeling tenotomyâ technique and reinserted, whenever possible, using nonabsorbable transosseous sutures with no tension and with the arm in a neutral position. A tenodesis of the long head of the biceps tendon to the pectoralis major tendon was performed if the long head of the biceps tendon was present.
All humeral implants were uncemented. The final humeral stem diameter corresponded to the number below the last probe used. The retroversion angle was set at 20° by aligning the version rod to the forearm. All humeral implants were in an onlay construction, with a reverse tray of 1-mm thickness and 1.5-mm offset at the â6â position using a polyethylene 36 insert and a final neck-shaft angle of 145°.
The glenoid baseplate was placed on the inferior margin of the glenoid rim, with ° of glenoid inferior tilt in standard RSA and 1° of glenoid inferior tilt in the BIO-RSA. For standard RSA, a 36-mm centered glenosphere and a baseplate with 25-mm diameter and a short 15-mm central post were used in all cases. The BIO-RSA technique involved harvesting a 10-mm-thick cylindrical autograft of cancellous bone from the humeral head as described by Boileau et al. [9]. A glenoid baseplate implant with 29-mm diameter and an extended 25-mm central long post was used to ensure host bone contact with the BIO-RSA, and a 36-mm centered glenosphere was used in all patients.
Postoperatively, the arm was placed in a sling for 4 weeks. Passive mobilization was allowed immediately after the operation. After 4 weeks, the sling was discontinued, and active ROM was initiated. Activities of daily living were allowed.
Baseline characteristics were age, sex, and limb dominance. All patients in both groups were examined postoperatively after at least 1 year by two orthopedic surgeons (AR and TAB) not involved in the surgery. The measured ranges of motion consisted of active forward elevation in the scapular plane, abduction, external rotation, and internal rotation. Strength was measured using a handheld dynamometer with the shoulder in neutral rotation and 90° of abduction in the scapular plane. Patients were asked to evaluate their pain (on a visual analog scale [VAS]), the Constant score [13], and to estimate their shoulder function as a percentage of a normal shoulder with the subjective shoulder value [14].
Radiographic and CT analyses were performed by two orthopedic surgeons (AR and TAB). No attempt was made to determine the reliability of the observations, and when differences in assessments were noted, the observers reached a consensus. The evaluation followed the model used by Boileau et al. [8]. On the glenoid side, radiographs and CT scans were examined for bone graft healing and bone graft viability, defined by absence of lucent lines at any level (baseplateâto-graft or graftâtoânative bone interface) and stable graft thickness over time; glenoid component fixation (stable: no evidence of radiolucency at the baseplate-bone interface or around the peg or any screw; at risk: >1 mm of circumferential radiolucency at the baseplate-bone interface or around the peg or any screw; or loose: either >1 mm of radiolucency around the baseplate-bone interface and around all screws or a shift in the position of the baseplate) (Fig. 2); inferior scapular notching according to Sirveaux et al. [15]; inferior glenoid osteophytes or spurs at the level of the pillar; postoperative glenosphere inclination measured with the RSA angle (between the glenosphere and a line perpendicular to the line of the supraspinatus fossa) and glenosphere inferior overhang according to the position of the glenosphere with the inferior rim of the glenoid. On the humeral side, humeral component fixation according to the grading system of Sperling et al. [16] and partial or total greater tuberosity resorption were measured.
Descriptive statistics were used to report demographic data. Results of categorical variables are presented as number of cases and percentage, while those for quantitative variables are mean and standard derivation (SD). The Kolmogorov-Smirnov test was used to test for a normal distribution for quantitative variables. The groups were compared using two-tailed Student t-test and Mann-Whitney test (quantitative variables) or Fisherâs and Pearsonâs chi-square test (qualitative variables). IBM SPSS statistics ver. 24 (IBM Corp.) was used for statistical analysis, and statistical significance was set at P<0.05.
During the period of study, 67 primary total shoulder arthroplasties were performed. Of those, 42 fulfilled the inclusion criteria and 34 had a CT control. Radiological analysis was performed in these 42 individuals. The mean follow-up period was 27.6 months (range, 12â48 months).
The results of clinical evaluation between standard RSA and BIO-RSA are described in Table 1. Among 42 surgeries, 11 (26.2%) were performed in men and 31 (73.8%) in women, with a mean age of 69 years (SD, 6.4). Twenty shoulders (48%) underwent BIO-RSA, and 22 (52%) underwent standard RSA. The BIO-RSA and RSA groups were similar regarding sex (P=0.592), mean age (P=0.781), and dominant side operated (P=0.845). No differences in global Constant shoulder score (CSS; P=0.884), VAS score, and subjective shoulder score were found between BIO-RSA and standard RSA. Regarding ROM, a significant difference was found for active internal rotation (P=0.038) and for passive external rotation (P=0.013), with better results in BIO-RSA. No other differences were found regarding strength of abduction (P=0.678), active forward flexion (P=0.338), active abduction (P=0.266), active external rotation (P=0.986), passive forward flexion (P=0.99), passive abduction (P=0.256), and passive internal rotation (P=0.093).
The results of radiologic assessment between standard RSA (n=18, 53%) and BIO-RSA (n=16, 47%) are described in Table 2. The notching rate was 28% (n=5/18) in the standard RSA group and 33% (n=6/16) in the BIO-RSA group, but the standard RSA group had more severe notching (grade 2) than the BIO-RSA group (P=0.039). No other significant difference was found. Regarding BIO-RSA, we verified graft healing and viability in all patients, along with preservation of the 10-mm thickness, meaning absence of graft reabsorption.
Muscle slackening of the remaining rotator cuff muscles in conjunction with reduced rotational moment arms in non-lateralized RSA is partly responsible for less favorable results in external and internal rotation compared with lateralized RSA in biomechanical [2,17] and in vivo studies [12,18].
We found no statistically significant differences in overall clinical scores (CSS and subjective shoulder value) between the two groups. Analysis of complications did not show any differences between the surgical methods.
In our study, patients with BIO-RSA presented better passive external rotational and active internal rotation compared with standard RSA. Concerning external rotation, our results are in accordance with the results of Greiner et al. [12]. Those authors found even better results when excluding patients with significant deterioration of the teres minor (fatty infiltration of grade 3 or greater). In addition, patients with BIO-RSA showed an improvement in active internal rotation. According to our surgical technique, for both groups, a primary tension-free subscapularis tendon closure was performed. The quality of the repaired subscapularis cannot easily be measured, and no conclusion was reached as to whether this difference may be related to the preserved biomechanical properties of the subscapularis in lateralized RSA. Other factors such as increased internal rotational moment arms of the latissimus dorsi and the pectoralis major muscle in lateralized RSA may also contribute to this difference [19].
In addition to the shoulder tendon condition , other factors may also play a role in the differences in rotational function between non-lateralized and lateralized RSA. First, the external rotation moment arm of the deltoid is decreased after non-lateralized RSA [2]. Second, the number of posterior or anterior deltoid fibers contributing to external or internal rotational movements decreases as a result of the medialized center of rotation. In addition, bony impingement in internal and external rotation is dependent on glenosphere position. Maximal impingement-free rotational capacity has been shown for inferior translation, inferior tilt, and lateralization of the glenosphere [20]. Contrary to our results, two groups previously found no differences in ROM between the two groups [10,11].
Regarding radiologic evaluation, CT suggested complete graft integration and viability in all patients of the BIO group after 12 months of follow-up. No statistically significant differences were found in loosening of the baseplate or humeral stem. In our study, the notching rate was 28% in the standard RSA group and 33% in the BIO-RSA group. However, we found a significantly larger proportion of patients with grade 2 Sirveaux et al. [15] scapular notching in the standard RSA group. Our results are in accordance with Athwal et al. [10], reinforcing that bony lateralization of the center of rotation in RSA reduces the rate of inferior scapular notching, although another similar study found no such difference between groups [11].
Overall, our scapular notching rate is below others reported in the literature [8,10]. Despite the use of humeral implants with a 145° angle, associated with higher rates of scapular notching, the position of the glenosphere with a very low position of the inferior rim of the glenoid (83% in RSA and 56% in BIO-RSA) was a factor of the lower notching rate.
This study had some limitations, including its retrospective nature, absence of preoperative clinical evaluation for comparison, and lack of author blinding to device type. Moreover, the clinical outcomes were limited to 1 year of follow-up, preventing determination of differences, such as graft osteolysis or loosening in the groups, in the long-term. Although we tried to achieve maximal standardization in lateralization by using the same glenosphere implant in every patient, differences in the resulting lateralization due to differences in the amount of glenoid reaming or bone quality of the graft cannot be excluded. Despite the limitations, we believe that this study adds clinically relevant and useful evidence, although more studies are needed.
NOTES
Author contributions
Conceptualization: TAB, AR.Data curation: TAB, AR. Formal Analysis: TAB, AR. Investigation: TAB, AR. Methodology: TAB, AR, HF, LHB, RC. Project administration: TAB. Resources: TAB. Validation: TAB, HF, L LHB, RC. Visualization: TAB, AR Writing â original draft: TAB. Writing â review & editing: HF, LHB, RC.
Fig. 1.
Radiographs of standard reverse (A-C) standard reverse shoulder arthroplasty (RSA) and (D-F) bony-increased offset-RSA.

Fig. 2.
Axial (A, B) and coronal (C) computed tomography scan cuts of bony increased-offset reverse shoulder arthroplasty. Note the healing and viability of the bone graft and its thickness, confirming the absence of bone resorption or lysis.
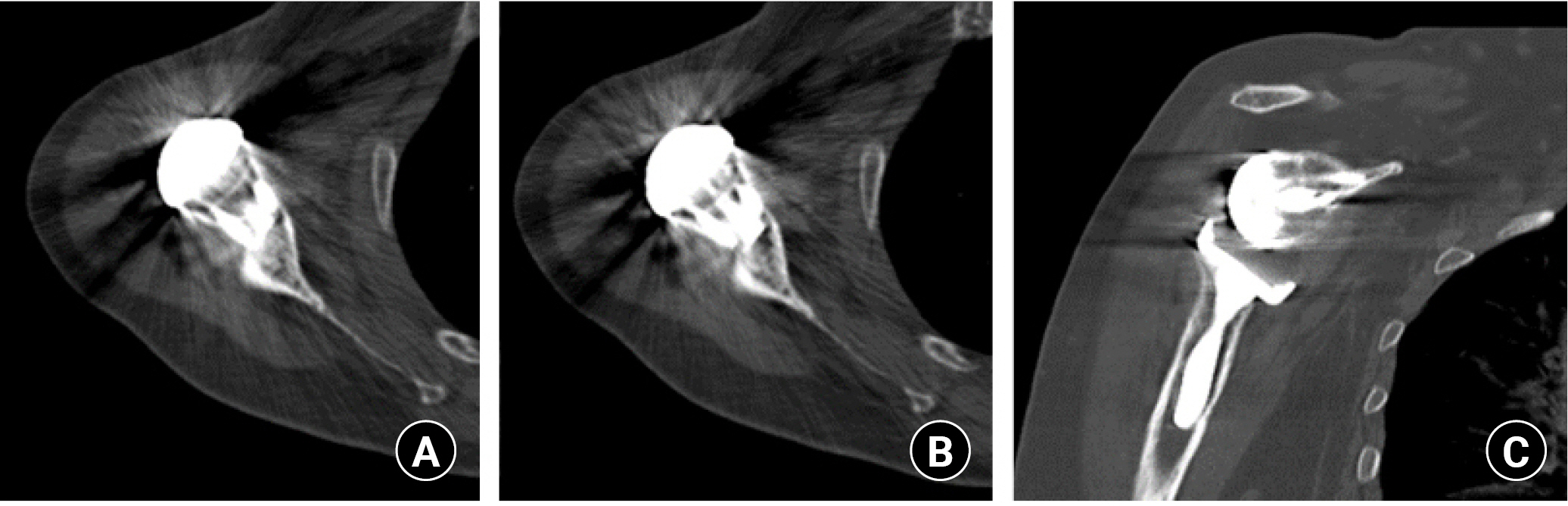
Table 1.
Results of clinical evaluation between standard RSA and BIO-RSA
Table 2.
Results of radiological assessment between standard RSA and BIO-RSA
| Variable | Standard RSA (n=18) | BIO-RSA (n=16) | P-value |
|---|---|---|---|
| Inferior scapular notching [15] | 0.038 | ||
| âGrade 0 | 13 | 10 | |
| âGrade 1 | 2 | 6 | |
| âGrade 2 | 3 | 0 | |
| Inferior glenoid osteophytes | 0.330 | ||
| âNo | 13 | 9 | |
| âYes | 5 | 7 | |
| Glenoid osteolysis | 0.105 | ||
| âStable | 14 | 16 | |
| âAt risk | 4 | 0 | |
| RSA angle (meanÂąSD) | 11.6Âą7.5 | 4.7Âą12.5 | 0.660 |
| Glenosphere inferior overhang | 0.210 | ||
| âFlush | 1 | 3 | |
| âLow | 2 | 4 | |
| âVery Low | 15 | 9 | |
| Humeral component fixation [16] | 0.108 | ||
| â0 | 14 | 15 | |
| â8* | 4 | 9 | |
| Greater tuberosity reabsorption | 0 | 2 | 0.214 |
REFERENCES
1. Tashjian RZ, Burks RT, Zhang Y, Henninger HB. Reverse total shoulder arthroplasty: a biomechanical evaluation of humeral and glenosphere hardware configuration. J Shoulder Elbow Surg 2015;24:e68â77.


2. Greiner S, Schmidt C, KĂśnig C, Perka C, Herrmann S. Lateralized reverse shoulder arthroplasty maintains rotational function of the remaining rotator cuff. Clin Orthop Relat Res 2013;471:940â6.



3. GutiĂŠrrez S, Comiskey CA, Luo ZP, Pupello DR, Frankle MA. Range of impingement-free abduction and adduction deficit after reverse shoulder arthroplasty: hierarchy of surgical and implant-design-related factors. J Bone Joint Surg Am 2008;90:2606â15.

4. GutiĂŠrrez S, Walker M, Willis M, Pupello DR, Frankle MA. Effects of tilt and glenosphere eccentricity on baseplate/bone interface forces in a computational model, validated by a mechanical model, of reverse shoulder arthroplasty. J Shoulder Elbow Surg 2011;20:732â9.


5. Werner BS, Chaoui J, Walch G. The influence of humeral neck shaft angle and glenoid lateralization on range of motion in reverse shoulder arthroplasty. J Shoulder Elbow Surg 2017;26:1726â31.


6. de Wilde LF, Poncet D, Middernacht B, Ekelund A. Prosthetic overhang is the most effective way to prevent scapular conflict in a reverse total shoulder prosthesis. Acta Orthop 2010;81:719â26.



7. Theivendran K, Varghese M, Large R, et al. Reverse total shoulder arthroplasty using a trabecular metal glenoid base plate: functional and radiological outcomes at two to five years. Bone Joint J 2016;98:969â75.

8. Boileau P, Morin-Salvo N, Bessière C, Chelli M, Gauci MO, Lemmex DB. Bony increased-offset-reverse shoulder arthroplasty: 5 to 10 years' follow-up. J Shoulder Elbow Surg 2020;29:2111â22.


9. Boileau P, Moineau G, Roussanne Y, O'Shea K. Bony increased-offset reversed shoulder arthroplasty: minimizing scapular impingement while maximizing glenoid fixation. Clin Orthop Relat Res 2011;469:2558â67.



10. Athwal GS, MacDermid JC, Reddy KM, Marsh JP, Faber KJ, Drosdowech D. Does bony increased-offset reverse shoulder arthroplasty decrease scapular notching. J Shoulder Elbow Surg 2015;24:468â73.


11. Collin P, Liu X, Denard PJ, Gain S, Nowak A, Lädermann A. Standard versus bony increased-offset reverse shoulder arthroplasty: a retrospective comparative cohort study. J Shoulder Elbow Surg 2018;27:59â64.


12. Greiner S, Schmidt C, Herrmann S, Pauly S, Perka C. Clinical performance of lateralized versus non-lateralized reverse shoulder arthroplasty: a prospective randomized study. J Shoulder Elbow Surg 2015;24:1397â404.


13. Constant CR, Murley AH. A clinical method of functional assessment of the shoulder. Clin Orthop Relat Res 1987;(214):160â4.


14. Gilbart MK, Gerber C. Comparison of the subjective shoulder value and the Constant score. J Shoulder Elbow Surg 2007;16:717â21.


15. Sirveaux F, Favard L, Oudet D, Huquet D, Walch G, MolĂŠ D. Grammont inverted total shoulder arthroplasty in the treatment of glenohumeral osteoarthritis with massive rupture of the cuff: results of a multicentre study of 80 shoulders. J Bone Joint Surg Br 2004;86:388â95.

16. Sperling JW, Cofield RH, O'Driscoll SW, Torchia ME, Rowland CM. Radiographic assessment of ingrowth total shoulder arthroplasty. J Shoulder Elbow Surg 2000;9:507â13.


17. Henninger HB, Barg A, Anderson AE, Bachus KN, Tashjian RZ, Burks RT. Effect of deltoid tension and humeral version in reverse total shoulder arthroplasty: a biomechanical study. J Shoulder Elbow Surg 2012;21:483â90.


18. Valenti P, Sauzières P, Katz D, Kalouche I, Kilinc AS. Do less medialized reverse shoulder prostheses increase motion and reduce notching. Clin Orthop Relat Res 2011;469:2550â7.



- TOOLS
-
METRICS

- Related articles in Clin Should Elbow
-
Complications of reverse shoulder arthroplasty: a concise review2021 March;24(1)







