Do partial glenohumeral degenerative changes in patients undergoing arthroscopic rotator cuff repair influence clinical outcomes?
Article information
Abstract
Background
The prognostic factors for patients with full-thickness rotator cuff tears (RCTs) include tear size, muscle atrophy and fatty infiltration. However, the influence of early coexisting degenerative changes on RCT outcomes is unappreciated. The purpose of this study was to calculate the impact that pre-existing partial glenohumeral cartilaginous changes have on patients undergoing arthroscopic RCT repair.
Methods
A study of 54 patients undergoing arthroscopic RCT repair was undertaken. The presence of co-existing patches of glenohumeral degenerative cartilaginous changes and RCT size was recorded at surgery. Pre- and postoperative outcomes were assessed using traditional (Oxford Shoulder Score [OSS], 5-level EuroQol-5D [EQ-5D-5L] questionnaire and EuroQol visual analog scale [EQ-VAS]) and patient-centric re-formatted prisms. Outcomes were assessed as an entire dataset, and sub-group analysis was performed according to the grade of co-existing arthritis and tear size.
Results
Significant improvements (p<0.05) in clinical outcomes were recognized when assessed using either the traditional or reformatted prisms (average % improvements in OSS, EQ-5D-5L and EQ-VAS were 47%, 33% and 43%, respectively; average improvements in pain, function, and psychological well-being were 48%, 33% and, 29%, respectively). Positive gain was noted in all sub-groups of arthritic grading and tear size.
Conclusions
Good clinical outcomes can be achieved following RCT repair even in the presence of local partial degenerative cartilage changes and advancing tear size. These benefits are patient-centered but require RCT repairability.
INTRODUCTION
Shoulder pain accounts for >2% of primary care consultations in the UK [1,2]. Full-thickness rotator cuff tears (RCTs) are the most frequent causes of shoulder pain and dysfunction, [3-5] accounting for 30%–70% of shoulder presentations. Non-traumatic RCTs become more common with age, with magnetic resonance imaging incidences of ≤13% in those aged <60 years and 28%–51% in those aged >60 years [6,7]. Most symptomatic RCTs when left untreated may progress in size, which can lead to rotator cuff arthropathy [8,9]. Numerous studies have reported surgical repair of full-thickness RCTs to be a highly effective treatment, providing significant clinical improvement with symptom and condition reversibility [10-14]. The management of end-stage rotator cuff arthropathy is more complex than that of a simple RCT when measured by any prism. Arthroplasty surgery carries a higher morbidity profile with less optimal outcomes compared to rotator cuff repair (RCR) as well as a notably higher fiscal cost of care [14,15]. Prevention is often preferred as a course of action over cure, and, with respect to the shoulder, if patients could be successfully diverted away from developing symptomatic end-stage glenohumeral arthritis, this would offer benefits to all from both population and socio-economic perspectives. However, the clinical burden that RCTs pose is likely to evolve inextricably and as a consequence of our aging population demographics [6,7].
Multiple patient and surgical factors concerning those with full-thickness RCTs already exist that provide accepted prognostic power. These include tendon tear size, muscle atrophy and fatty infiltration [8,9,16,17]. The prognostic impact of the presence of partial patches of degenerative arthritic and cartilaginous change is less appreciated. Osteoarthritis is not a binary disease; rather, it exists initially in progressive states [18]. It is not uncommon to note such partial degenerative changes in the glenohumeral joint at arthroscopy, and these findings are more common in patients as their age increases. In the presence of bone-on-bone end-stage arthritis, the surgical management of an RCT alone is not expected to offer an appropriate clinical benefit. What is less clear is the influence of early co-existing patches of degenerative change on RCR outcomes.
The purpose of the study was to calculate the impact that pre-existing glenohumeral cartilaginous change may have on patients undergoing arthroscopic repair of full-thickness RCTs. The working hypothesis was that such degenerative changes may inhibit end-outcomes.
METHODS
The study followed the requisite institutional requirements and advice and was approved by the Institutional Review Board. And, despite the retrospective design of this study, patient consent was attained. A retrospective analysis of consecutive patients undergoing arthroscopic RCR by consultant surgeons was performed over a 4-year period. Inclusion criteria were patients with symptomatic full-thickness RCTs who had failed conservative treatment. Patients were excluded if they had a prior history of shoulder surgery, obvious bone-on-bone glenohumeral changes on plain radiographs, an acute traumatic RCT, lacked suitable biology for healing, required additional subscapularis repair, required additional biceps tenodesis, had undergone previous cervical spine surgery or had a history of regional infection or a complex medical history with an American Society of Anesthesiologists classification of ≥4 [19]. Additionally, if patients had patches of bone on bone progressive cartilaginous degenerative changes measuring >1 cm by >1 cm at arthroscopy, they were also excluded. All patients underwent clinical cervical spine review. If patients had active and concomitant cervical symptoms with radicular symptoms, they were also excluded.
Arthroscopic surgical repair was performed under a general anesthetic with the patient in the beach chair position. All patients underwent surgery at the same orthopedic elective center, undergoing preoperative work-up performed by the same teams, surgery from the same surgeons and the same postoperative physiotherapy regimes. All RCTs were repaired using an all-arthroscopic technique.
At arthroscopy, the size of RCT and the presence of any coexisting patches of glenohumeral degenerative cartilaginous change were recorded. Cartilage changes were graded using the Outerbridge classification [18], which is based on direct visualization of the joint and was developed to be a reproducible methodology to grade changes to articular cartilage. The system assigns a grade of 0–4 to the chondral area of interest, where grade 0 suggests normal cartilage, grade 1 suggests cartilage with softening and swelling, grade 2 suggests a partial-thickness defect with fissures on the surface that do not reach subchondral bone, grade 3 suggests full-thickness fissuring to the level of subchondral bone and grade 4 suggests exposed fully subchondral bone.
Additional findings recorded at surgery included the RCT size, the number of anchors used in repair and the stability of the repair during range-of-movement examination and additional procedures (e.g., arthroscopic acromioclavicular joint decompression). The footprint of the greater tuberosity was prepared prior to repair. A complete repair of the full-thickness RCT was conducted, which returned the tendon to cover the entirety of the greater tuberosity footprint with a double-row repair technique utilizing triple loaded 5.5-mm Healix anchors (Depuy Mitek, Raynham, MA, USA) in a double-row repair approach. Those patients with cuff tears >2 cm required two anchors to achieve this, whilst those with smaller tear patterns only required one anchor. In the latter group, two more medially placed mattress sutures were initially tied and a subsequent lateral simple suture was completed. In those with two anchor repairs, two to three more medially placed mattress sutures were secured initially, followed by two simple sutures, to a more laterally placed anchor. Following surgery, patients were immobilized in a sling for 4 weeks before commencing full range of movement and a structured active assisted exercise program.
Outcomes
Clinical outcomes were measured using standard patient-reported outcome measures, including the Oxford Shoulder Score (OSS), the 5-level EuroQol-5D (EQ-5D-5L) questionnaire and the EuroQol visual analog scale (EQ-VAS) [20,21]. The OSS is a subjective patient-based questionnaire used to assess shoulder pain. It asks 12 questions, each with five potential answers, covering pain and functional disability. The OSS was specifically designed as a research tool to assess outcomes following shoulder surgery; however, it does not provide more holistic information. The EQ-5D-5L and EQ-VAS are also subjective scoring systems assessing some of these more holistic aspects of care, including treatment expectations, patient perception, satisfaction and anxiety and depression.
Outcome assessments were performed preoperatively and ≥6 months postoperatively. To translate the data into a more patient-centered format, a validated matrix formula was applied [14,22]. The three outcomes tools were converted to have a uniform scale, where positive and negative findings shared the same polarity. In total, the outcome score included values added from 20 questions that formed the basis of the tier two outcomes [23,24]. These questions were re-formatted into questions relating to the three domains of pain, function and psychological and secondary health markers, which were mathematically converted to a uniform score out of 100 points, where 0 points represented the worst outcome possible and 100 points represented the best. The scores for each of the three domains could then be summed to form an aggregate score out of 300 points. The percentage change between a patient’s preoperative and postoperative outcomes was then compared across each separate domain to determine the summed score percentage change. Outcomes were assessed as an entire dataset and sub-group analysis by grade of co-existing arthritis and tear size.
Statistical Analysis
Chi-square testing was used to assess the relationship between nominal categorical variables. Mann-Whitney-Wilcoxon testing was performed to assess the relationship between continuous non-parametric data (OES, EQ-5D-5L and EQ-VAS scores). A p-value of 0.05 or less was considered statistically significant.
RESULTS
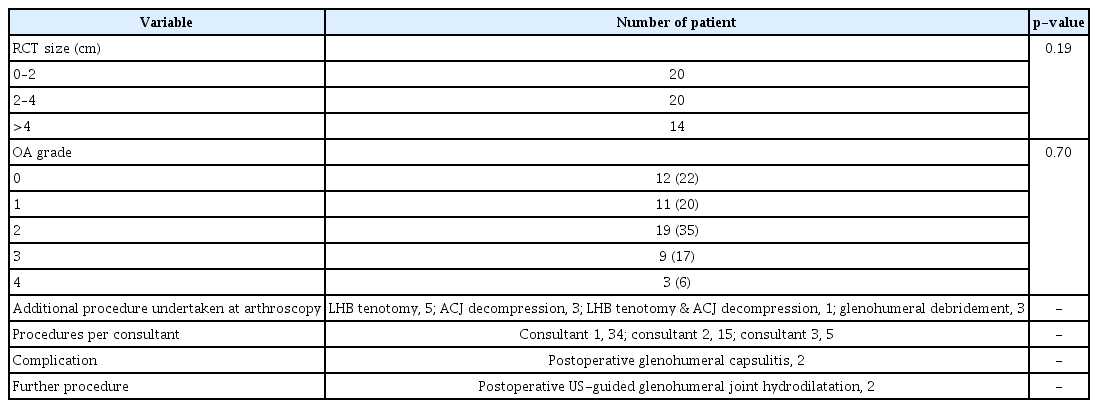
This study included 54 patients (20 men and 34 women) with an average age of 61 years (range, 41–81 years). A variation in tear sizes was noted in the cohort, with less massive tears dominating; however, there was no significant imbalance between the groups (Table 1). The observed spectrum of rotator cuff pathology in this study was in keeping with most general shoulder practices. Similarly, there was variation in coexisting patches of glenohumeral degenerative cartilaginous changes (Table 1). When the size of the tear was compared against the grade of pre-existing degenerative change, it was noted that the smaller tears (<2 cm) more frequently had less progressive cartilaginous changes (grade 0 or 1) compared to those with larger RCTs (Table 2). Conversely, those with the greatest RCT size (>4 cm) had significantly more progressive cartilaginous changes (grade 3 or 4) compared to those with smaller RCTs (p=0.03).
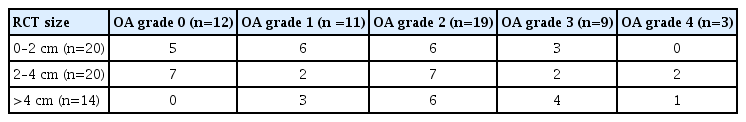
Patients categorized following comparison of arthroscopic findings (grade of pre-existing cartilaginous degenerative change against the size of RCT)
The average duration for follow-up was 19 months (range, 6–27 months). The average range of movement at discharge regarding forward flexion was 166° (range, 80°–180°) and abduction was 162° (range 70°–180°), respectively. A low rate of complications was observed (n=2/54, 3%), and both complications related to postoperative capsulitis and both patients had a successful outcome following ultrasound-guided glenohumeral joint hydrodilatation (Table 1). No other subsequent procedures were performed on the operated shoulders.
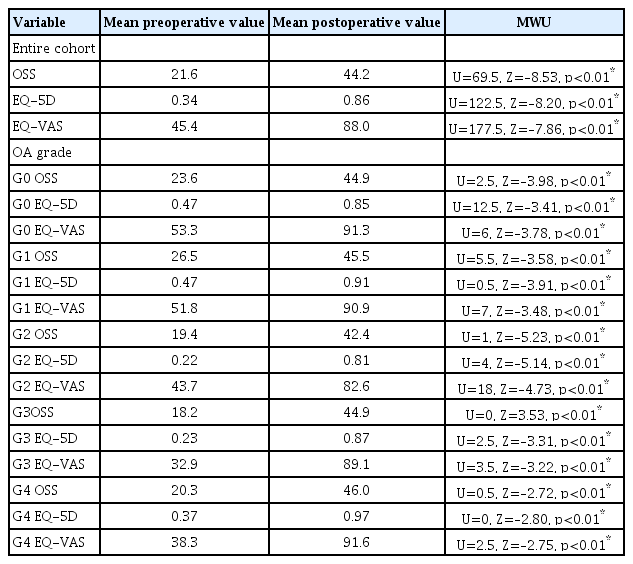
When the whole-cohort clinical outcomes were assessed using the OSS, EQ-5D-5L questionnaire, and EQ-VAS, a significant improvement (p<0.05) were recognized (Tables 3 and 4). This was noted when values were analyzed by either the traditional or re-formatted scoring measures (Table 5). When the outcome measures were reorganized to assess the domains of pain, function and psychological well-being, there were significant improvements recorded; however, this was accompanied by some variation at the patient level, with not all patients uniformly seeing improvement in all domains (Figs. 1 and 2).
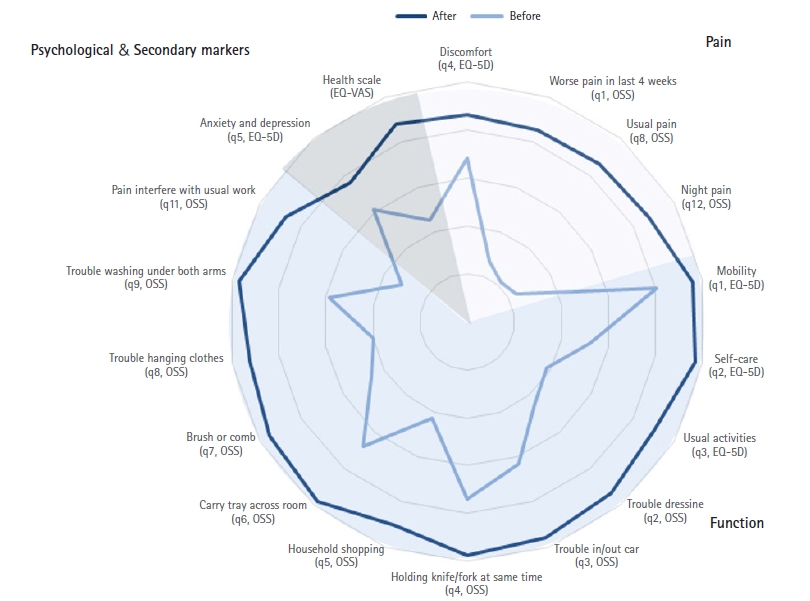
Radar graph displaying the changes in response to individual patient-related outcome measure (PROM) questions before and after surgery. The Oxford Shoulder Score (OSS), 5-level EuroQol-5D (EQ-5D) questionnaire, and EuroQol visual analog scale (EQ-VAS) values were re-formatted to present a patient-centric representation of PROMs before and after rotator cuff repair surgery. q: question.

Change in outcome following rotator cuff repair surgery from a better versus worse perspective compared to the individual patient’s preoperative state as measured by the Oxford Shoulder Score (OSS). OA: osteoarthritis (graded by the Outerbridge classification).
A sub-group analysis of outcomes by pre-existing degenerative changes indicated that preoperative scores were not significantly different independent of the grade of degenerative change. There was a significant improvement within individual sub-groups compared to between pre- and postoperative scores (p<0.05). However, there was no notable difference in end-outcome scores amongst the different grades of cartilaginous degenerative changes (p>0.05). Patients were additionally assessed from the perspective of whether their end-outcomes were better or worse than their presenting position, and their relative changes, being either positive or negative, were individually plotted on a line of best fit (Fig. 2); ultimately, almost all results were on the positive side of the line of fit, indicating an improvement in their condition. However, there was an element of variance in outcomes, with not all patients having the same experience.
Sub-group analysis of outcomes by RCT size indicated that preoperative scores were not significantly different independent of RCT size (p>0.05). There was a significant improvement within individual sub-groups compared to between pre- and postoperative scores (p<0.05). However, there was no significant difference in end-outcome scores amongst the different classes of RCT size assessed.
DISCUSSION
This study has demonstrated that good clinical outcomes can be achieved following RCT repair even in the presence of local partial degenerative cartilaginous changes and advancing RCT size. As such, the hypothesis that pre-existing degenerative changes would inhibit end-outcomes has not been proved. The described clinical outcome benefits are patient-centered but require RCT repairability. The data presented indicate a positive gain independent of the grade of partial degenerative cartilaginous changes. However, the achieved improvements in outcomes were not universal and did not routinely return the individual to complete normality (Table 3 and Fig. 2). Rather, RCR surgery led to a significant positive change in outcomes that had meaning to the patients with respect to the domains of pain, function and psychological well-being (Table 5).
It is accepted that the surgical management of symptomatic RCTs is a high-value care intervention [14]. Previous randomized controlled trials assessing the management of patients with surgical repair of RCTs versus non-surgical care strategies had to be halted and adapted because of high cross-over rates for those in the non-surgical arms subsequently requiring surgical fixation [11]. If those with symptomatic RCTs are neglected, the scenario can deteriorate and increase the risk of progression toward a classical rotator cuff arthropathy picture [8,9,16,17,25]. Such a situation is more complex to manage and is associated with less favorable end-results compared to the management of a simple RCT. Many would agree that avoiding the potential morbidity of arthroplasty if possible is an attractive goal. National guidelines suggest arthroplasty is rarely the first-line treatment option [26]. The financial costs of arthroplasty are also high compared to arthroscopic RCR [14,15].
Whilst the presentations of a conventional uncomplicated RCT and that of a rotator cuff arthropathy are markedly different, they are on the same continuum of disease. Generally, the concept of delaying or reversing disease progression is attractive if possible, and such logic is accepted when offering RCR to patients. In turn, RCR is noted to be a high-value intervention [14]. The demographic of patients with symptomatic RCT is similar to those that may be developing partial degenerative cartilaginous changes. Local partial progressive cartilage changes are often noted at arthroscopy. A reasonable working hypothesis could be that the end-outcomes of RCR may be less optimal in the presence of florid progressive degenerative changes; however, the impact of limited patches of change are less well appreciated.
The results in this study have demonstrated positive alterations in all groups of partial degenerative changes, although there were a limited number of patients enrolled with patches of grade 4 cartilaginous changes, so the data should be interpreted judiciously. It must be noted that those who did exhibit grade 4 changes had small discrete patches of change only. The presence of such progressive changes was not expected prior to surgery, and the patches themselves were very limited. As such, these patients did not represent a classical rotator cuff arthropathy picture. Patients with florid grade 4 changes were not considered. Arthroscopic RCR is not the advocated treatment in those with gross widespread bone-on-bone glenohumeral degenerative changes, and such presentations were excluded in this study [26,27]. Interestingly, however, the data showed similar levels of improvement following RCR in patients with other grades of partial cartilaginous changes. The data also indicated a correlation regarding the presence of more advanced grades of cartilage changes in those with larger RCTs. This finding is in keeping with existing experiences. The notable benefit of RCR to such patients is likely linked to the reactivation of the rotator cuff couple and biomechanical axis of action [28,29]. This in turn promotes stabilization of glenohumeral movement whilst attenuating eccentric high-energy glenohumeral loading. This theoretically could inhibit further cartilage misloading or injury. The evidence for this in the glenohumeral joint is limited, but the concept of restoring the mechanical axis to protect the joint is well established in other joints, with osteotomy surgery being an example of how this theory is clinically enacted [30]. Following RCR, patients enjoy heightened success if they have factors in favor of repairability [16]. As such, a nuanced surgical decision-making process is crucial, and offering RCR to patients in the absence of such positive characteristics may not lead to such a successful outcome.
Analyzing the degree of failure or success following an intervention can be challenging. Objective classical scoring measures, such as OSS, offer potential solutions with absolute scores. Such scores in isolation fail to express the degree of change delivered by the treatment and may lack real-world relevance to the patient. The current study assessed outcomes using traditional and re-formatted measures that can be readily interchanged. Previous works have highlighted the patient-centered benefits when using outcomes that are easily intelligible and relevant to patients [14,22]. Within this study, this approach helped to highlight the notable improvements in those who had more progressive cartilaginous change or larger-sized RCTs. This may reflect the fact that they enjoyed a greater potential uplift from a poorer starting point and, in turn, this considerable improvement in their biomechanical action triggered a meaningful change in their symptoms.
This study has several obvious limitations, which include the limited number of patients in the study and the fact that the patient sub-groups were unmatched in number or demographics. There is no long-term follow-up data of this group currently available, and it is possible that some of the patients may experience disease progression, requiring additional treatment. Given that the patients assessed had demonstrable cartilaginous changes, it is possible that, over time, some of these patients may require arthroplasty. This study can provide no estimation of the number or sub-groups that might trend to this point. The enrolled patients did not undergo routine postoperative imaging to evaluate the RCR. This is not part of the unit’s standard practice and, as such, this present study cannot conclusively report on cuff integrity; however, outcomes were assessed clinically in keeping with accepted national practice. This study was undertaken at a single center by a limited number of surgeons. However, there was a shared management philosophy and surgical technique amongst the surgeons that enhanced the standardization of the treatment pathway. The re-formatted outcome prisms were unequally weighted, specifically regarding the assessment of psychological well-being. We would expect that future revisions would require this domain of analysis to be expanded and directed by patient-derived measures.
In conclusion, this study provides evidence that good clinical outcomes can be achieved following RCT repair, even in the presence of local partial degenerative cartilage changes and advancing tear size. These benefits are patient-centered but require RCT repairability. We advise that patients undergo careful selection, especially if more advanced patches of degenerative change are suspected in combination with larger-sized RCTs. Repairing the symptomatic RCT patient before they convert to a rotator cuff arthropathy can offer potential salvage and, as such, is a high-value intervention. We recommend that RCR should be considered following appropriate review in those with biological repairability, even in the presence of partial glenohumeral degenerative changes.
Notes
Financial support
None.
Conflict of interest
None.